
Is Vicky Pattison speaking out on PMDD a call for action?
Many women feel like there should be more awareness for gynaecological conditions, as Vicky Pattison speaks out on her PMDD diagnosis.
Former Geordie Shore star Vicky Pattison recently appeared on ITV’s Good Morning Britain to discuss her premenstrual dysphoric disorder (PMDD) diagnosis earlier this year. She spoke about how this led to her not feeling herself, not wanting to see her friends and family and even her having suicidal thoughts. According to the Royal College of Nursing 5 to 8% of all menstruating women are diagnosed with PMDD and several of these can be misdiagnosed, such as for conditions like depression.

Image credit – Alamy
Vicky Pattison spoke in the Houses of Parliament about women’s reproductive health, along with her own experience, as IAPMD research shows diagnosis can take an average of 12 years, yet some women report to suffer with symptoms for up to 30 years.
Dr Sarah Cooke, GP and Registered Associate Nutritionist, said: “Women experiencing PMDD can have severe mood changes in their cycle – often seven to ten days prior to their period – and sometimes these mood changes can lead to suicidal thoughts or making big decisions, such as quitting their job or breaking up with their partner.
“At other times in their cycle they do not generally have these thoughts which can make the sudden change feel more distressing. Treatment for PMDD may be similar to anxiety or depression, but there may be other options to explore which require a correct diagnosis.”
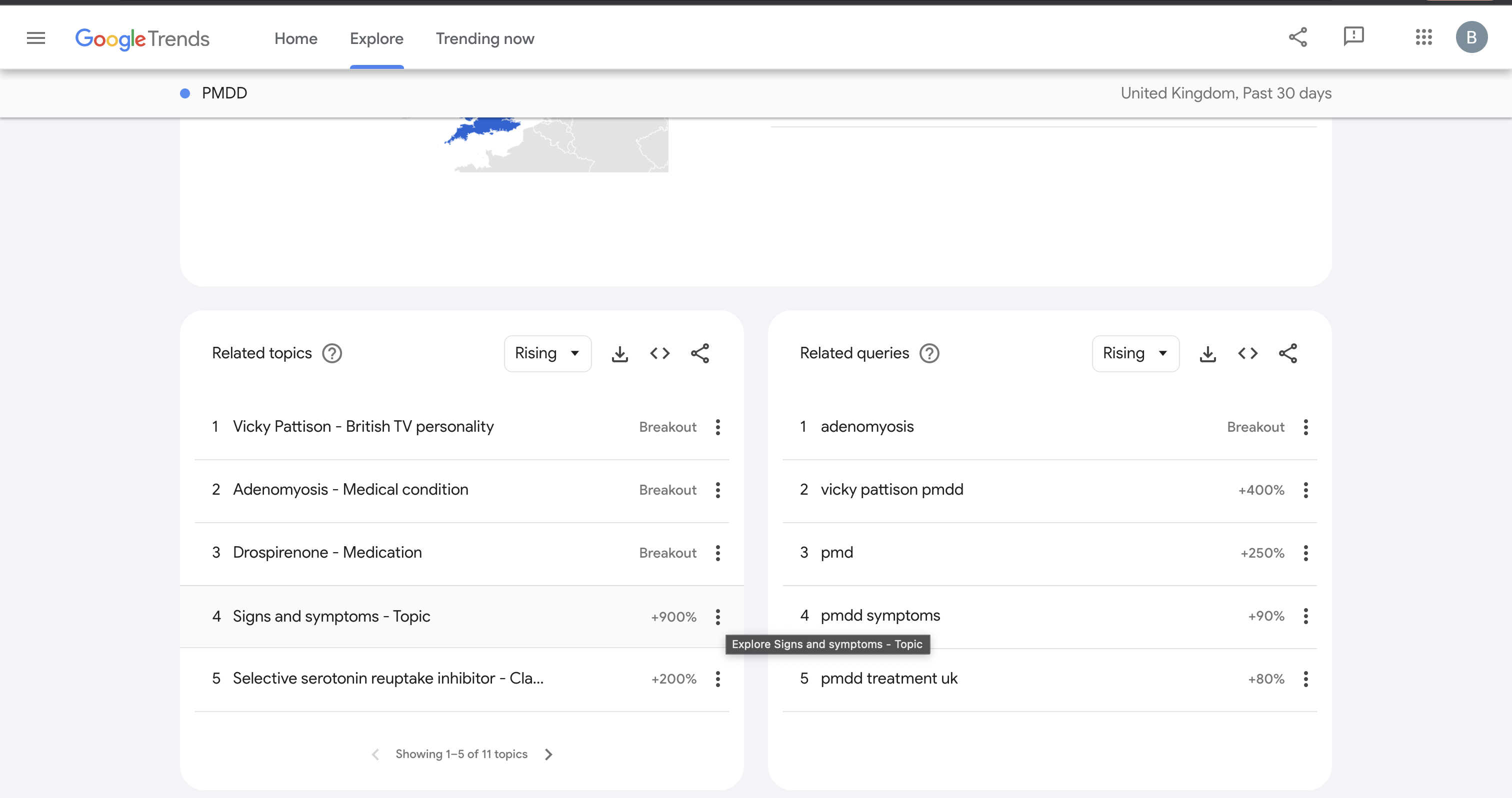
Google trend searches of PMDD in the last 30 days
Aside from PMDD, there are several other gynaecological conditions, such as polycystic ovary syndrome (PCOS) and endometriosis that women suffer from on a daily basis. In the Department for Health and Social Care’s (DHSC) Women’s Health survey, published in 2022, they found that less than one in five respondents have enough information on menstrual wellbeing (17%) and less than one in ten have enough information on the menopause (9%) and gynaecological conditions (8%.)
Some of the solutions that respondents put forward were to improve the quality of information available to the public and improving and expanding the education of healthcare professionals.
Georgina Sturmer, counsellor and MBACP, said: “Conditions that are associated with women’s health are often referred to as being invisible. This isn’t because they are peaceful or benign. It’s because of the stigma that our society has attributed to them and the lack of information, or sometimes conflicting information, that we have.
“When we suffer from a painful condition like PMDD or endometriosis. It can make it even harder for us to feel happy in our own skin. We might feel frustrated or angry about the pain and uncertainty that we have to live with.”
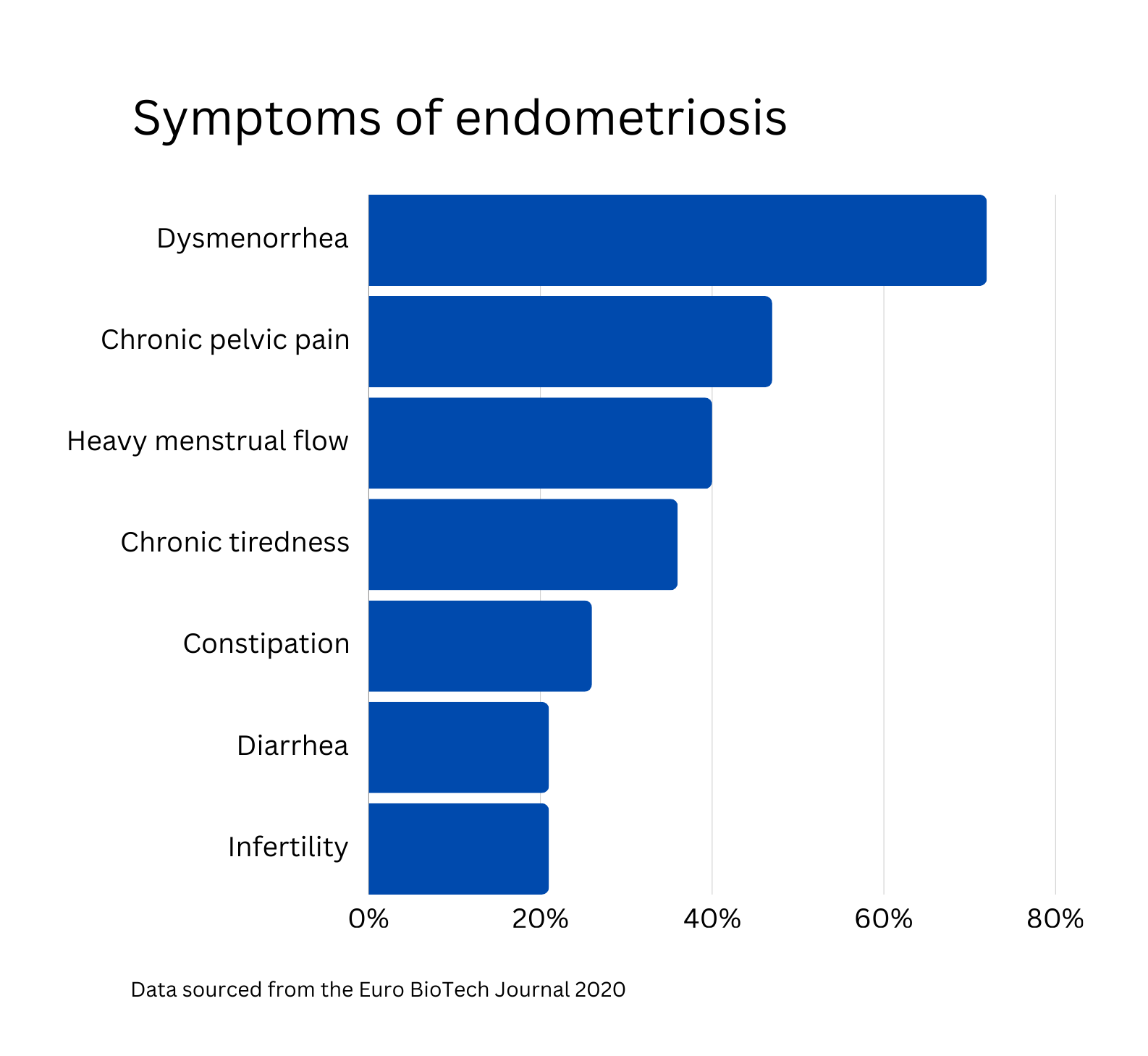
According to Endometriosis UK, 10% of women worldwide have endometriosis, which is 176 million and it is the second most common gynaecological condition in the UK. It’s a condition where tissue similar to the uterus lining grows outside the uterus and this can lead to lower tummy or pelvic pain and can ultimately lead to difficulty becoming pregnant or even infertility.

Courtney Henderson, Council worker, was diagnosed with endometriosis in March 2023, but has suffered with symptoms since the age of 14. She said: “I remember passing out at school due to the pain and realising this was not just normal period cramps. I have also experienced extreme fatigue, back pain and abdominal pain for the past ten years.
“It affected my life massively, some days vomiting and passing out from the pain and some days not even being able to leave my bed, missing school, college, work and social events.”
In the 2022 Women’s Health Strategy for England survey more than 84% of women said they felt at times that their healthcare professionals were not listening to them. Courtney added: “I first went to my GP when I was 15 and was told my period pain was normal for all women and to take paracetamol. I was told the exact same thing over and over again in multiple appointments and that I was overreacting. It felt like nobody was listening to how much pain I was in, or they didn’t believe me.
“In 2022 I visited my GP again, explaining my research into endometriosis. Finally, the first female GP I had seen in the ten years agreed with me that the level of pain and the symptoms I was experiencing wasn’t normal. Around six months later I had a laparoscopic surgery and they did find endometriosis and scar tissue.
“I have found useful and informative support groups on Facebook and I would urge anyone experiencing symptoms of endometriosis to not be afraid to advocate for yourself. Don’t be afraid to push for more tests and investigations if you are not being listened to.”
Endometriosis costs the UK economy £8.2 billion a year in treatment, loss of work and healthcare costs according to Endometriosis UK, however the cause is unknown and there is no definite cure. Treatments can include anti-inflammatories such as ibuprofen, hormone treatments like contraceptive methods or surgery, which can be used to remove or destroy areas of endometriosis tissue to improve symptoms.
While there are women out there gaining the diagnosis and help they require, there are still a number who are suffering, which is why awareness needs to be spread for gynaecological and other women’s health conditions.

